Repealing Florida Statute §768.21(8) and Restoring Medical Accountability
Executive Summary: Florida Statute §768.21(8) has been the subject of public debate for more than three decades. Much of that debate has focused on whether certain families should be permitted to recover non-economic damages in medical negligence wrongful death cases. While this issue raises important questions of fairness, it also reflects a deeper policy challenge involving how Florida’s legal, medical, and regulatory institutions respond when serious medical errors occur.
This project examines the full history of Florida’s wrongful death laws—from its nineteenth-century origins to the 1972 reforms and the medical malpractice crisis of the 1980s—and explores how those developments produced the current statutory framework. Rather than approaching the issue solely through the lens of litigation.
The Accountability Gap framework presented here invites policymakers to consider a broader systems approach that balances transparency, accountability, patient protection, and the long-term stability of Florida’s healthcare system.
The Accountability Gap describes a structural failure: a gap is created when preventable medical deaths occur, but systems fail to acknowledge errors, assign responsibility, and implement corrective action. Florida Statute §768.21(8)—a subsection of Florida’s Wrongful Death Act—widens that gap by restricting which surviving family members may recover non-economic damages in a defined class of wrongful death cases. The statute does not change the medical standard of care, and it does not “legalize” negligence. Its effect is practical: by removing the category of damages that often makes complex medical negligence cases economically feasible to litigate, it frequently prevents these cases from ever reaching the civil justice system, the one mechanism that consistently compels discovery, public fact-finding, and institutional feedback after a serious medical failure.
Our current efforts to repeal §768.21(8) are based on the belief that the statute weakens equal access to accountability, disrupts patient-safety feedback loops, and erodes public trust in the fairness of Florida’s wrongful death framework. Bridging that gap is the purpose of this initiative.
What §768.21(8) Is
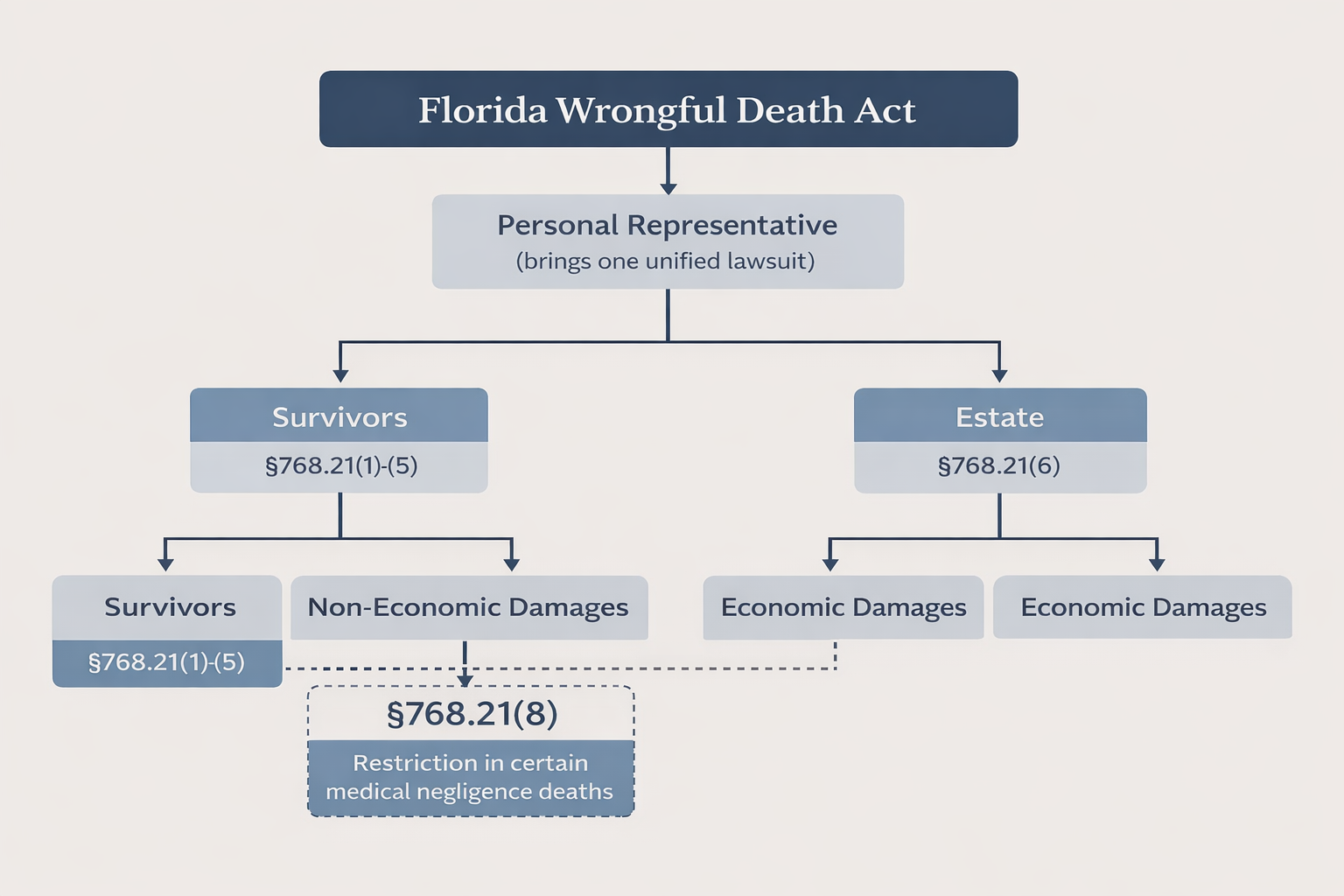
Florida’s Wrongful Death Act governs who may bring a wrongful death claim and what damages may be recovered when a person dies due to the wrongful act or negligence of another. Within that framework, §768.21(8) limits the availability of non-economic damages—commonly understood as damages for mental or emotional pain and suffering and the loss of companionship, instruction, and guidance, for certain survivors in certain circumstances.
In plain terms, the statute creates a category of wrongful death cases in which the survivors most directly harmed by the death, the immediate family members, may recover only economic damages (such as medical bills and funeral expenses) but are barred from recovering the non-economic losses that normally reflect the human realities of death: grief, loss of companionship, and the deprivation of a family relationship.
This is not a theoretical distinction. Non-economic damages are often the only damages that make medical negligence wrongful death cases economically feasible to litigate, because these cases are expensive to investigate and prove. They require specialized expert review, complex medical causation analysis, and substantial litigation costs. When the recoverable damages are restricted to economic losses alone—often modest or minimal in the context of death—many cases become practically impossible to bring, regardless of the strength of the underlying negligence.
The result is predictable: a significant number of preventable deaths never reach a courtroom, never reach a jury, and never receive the level of scrutiny that civil litigation uniquely provides. Further, due to the difficulties grieving families encounter when filing a claim of negligence with Florida’s regulatory agencies, i.e., the Department of Health or the Agency for HealthCare Administration, these potential cases are never brought to the attention of the Boards of Medicine and Nursing.
What the Statute Does in Practice
Many people assume that accountability after medical negligence is inevitable—that if a preventable death occurs, the facts will be investigated and the responsible parties will be held accountable. In reality, accountability depends on whether the systems designed to reveal facts and impose consequences are allowed to operate.
In Florida, civil litigation has historically served as the primary mechanism for producing that result. Lawsuits compel disclosure. They force the production of medical records. They require sworn testimony. They allow independent medical experts to evaluate whether the standard of care was met. They allow cross examination of both plaintiff and defendant. And they allow a neutral decision-maker—often a jury—to determine whether negligence occurred and what consequences should follow.
When §768.21(8) renders litigation financially infeasible, that mechanism often disappears, particularly when economic damages alone are not enough to finance the case. Families are then pushed toward administrative complaint pathways—such as filing complaints with the Department of Health or other agencies—which are not designed to provide the same kind of public fact-finding, discovery, or systemic feedback.
Administrative oversight has an important role. Licensing boards such as the Department of Health and the Agency for HealthCare Administration can impose discipline. These Agencies can investigate professional conduct. But these processes are typically opaque to the public, procedurally narrow, and limited in scope. They are not structured to answer all the questions families have after a death, and they are not designed to create the same kind of broad institutional accountability that civil litigation can produce.
The practical effect of §768.21(8) is therefore not merely a reduction in damages. It is often the elimination of the only pathway that reliably exposes what happened and compels correction.
Why Repeal Matters
This initiative is not driven by a desire to punish physicians or destabilize Florida’s healthcare system. It is driven by a systems-based recognition: when accountability mechanisms are selectively disabled, preventable errors are more likely to persist.
A functioning civil accountability system does more than compensate families. It creates an external feedback mechanism that forces institutions to confront errors. It exposes weak policies, documentation failures, communication breakdowns, and patterns of preventable harm. Even when cases settle, the process itself often drives internal review and corrective action precisely because the risk of public adjudication requires attention and reform.
When §768.21(8) prevents these cases from being brought, the system loses that external pressure. The public loses visibility. Regulators may never receive a complete picture. And hospitals and providers may not face the same structured incentives to identify and correct the conditions that led to the harm in the first place.
In short, the statute creates a measurable gap between harm and accountability.
The Accountability Gap as a Public Policy Problem
Florida’s medical negligence debate is often framed as a conflict between families and healthcare providers, or as a question of money. That framing misses the deeper issue. This is a public policy problem concerning the structure of accountability.
The law should be built to do at least three things after preventable medical harm:
Reveal the truth about what occurred.
Assign responsibility where standards were breached.
Drive corrective action so the same preventable harm is less likely to recur.
When a statute forecloses the primary mechanism capable of doing those things in a transparent, structured way, the system becomes less reliable, not only for injured families, but for patient safety generally.
This is also an equal-justice problem. Florida’s Wrongful Death Act does not impose these restrictions uniformly. It draws lines between categories of survivors, meaning that the availability of accountability can hinge on family status rather than the severity of negligence or the preventability of death. When legal remedies are distributed unevenly, confidence in the fairness of the system erodes. People begin to believe—often with good reason—that some deaths receive scrutiny and others do not.
Public trust is not maintained by slogans. It is maintained when systems consistently behave in ways citizens recognize as fair.
What We Are Doing
Our current efforts are aimed at documenting, explaining, and correcting the structural effects of §768.21(8). This work includes:
explaining what the statute does and how it reshapes the accountability landscape after medical negligence deaths;
analyzing the history of how and why the statute was enacted and maintained;
examining how the civil justice system, regulatory systems, and healthcare risk environment interact;
proposing reforms that restore meaningful accountability while respecting the legitimate concerns of healthcare providers and the economic realities of medical risk.
Repeal is not the end of the conversation; it is the beginning of a more functional one. If Florida restores civil accountability to the class of cases currently affected by §768.21(8), policymakers must still consider the broader system: how professional discipline operates, how adverse events are disclosed, how medical errors are corrected, and how public safety is protected without destabilizing healthcare access.
Repeal is a necessary first step as it restores the public’s access to the only mechanism that consistently brings the facts into the light.
Where This Page Leads
This page serves as an introduction. In the sections that follow, we will provide deeper explanations and supporting materials, including:
a plain-language breakdown of §768.21(8);
the legislative history and major turning points in Florida’s medical liability debate;
a comparison of civil litigation and administrative oversight as accountability mechanisms;
policy options that restore accountability while addressing risk and stability concerns.
The Accountability Gap is not a slogan. It is a description of what happens when preventable medical deaths occur and the systems designed to respond cannot—or do not—function as they should.
Our goal is to close that gap.

Click The Links Below To Explore This Topic Further
The sections below trace the history of Florida’s wrongful death laws and the policy decisions that shaped today’s debate over accountability in cases of medical negligence.
The Foundation: Understanding the law itself
The Road to Subsection (8): How the law came into existence
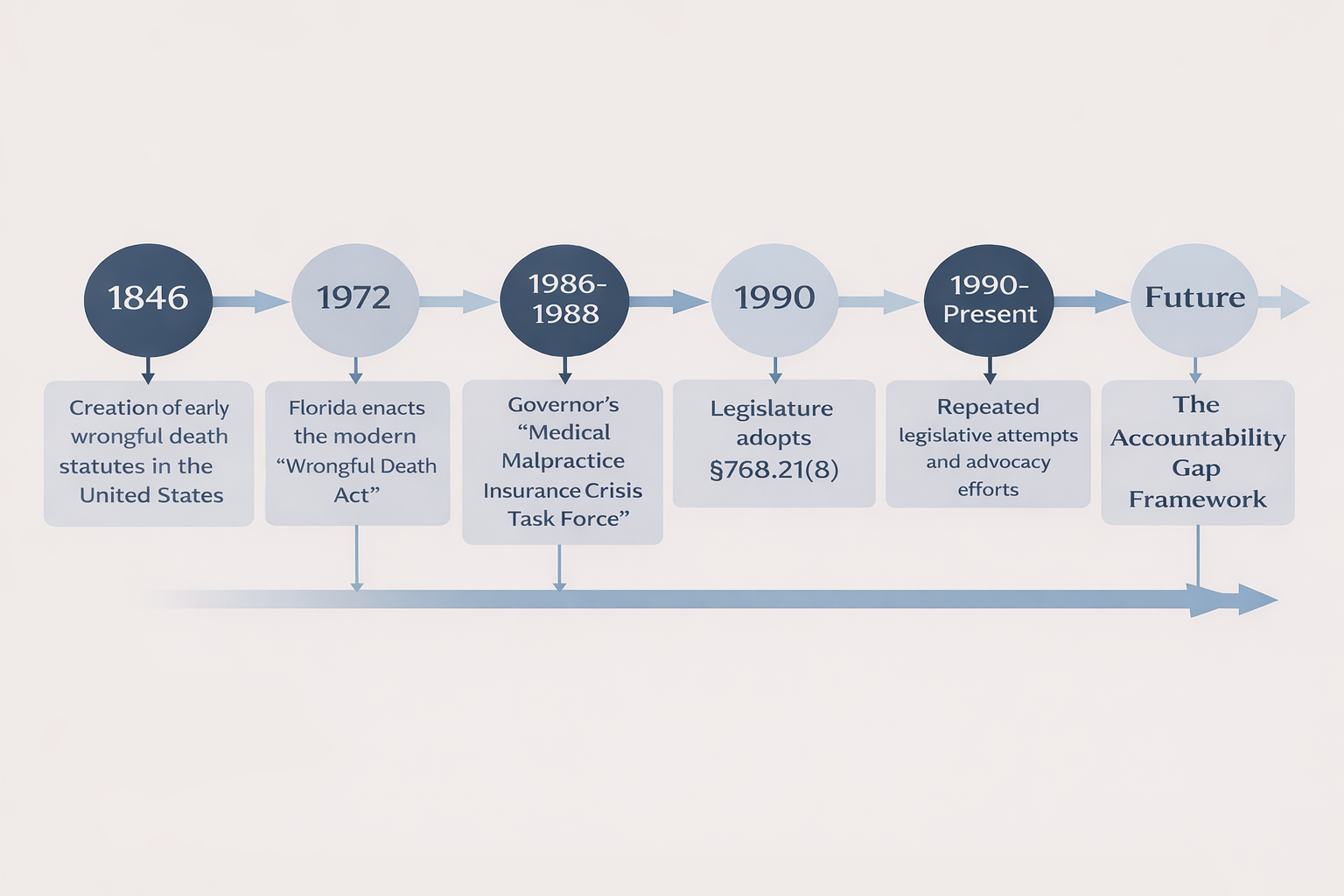
The Road to Repeal Subsection (8):
Modern developments and reform